10 minute read
Takeaway: Comparing organisations is not as simple as identifying one company’s good practices and then copying and pasting over your organisation.
The UK Health Secretary, Matt Hancock, was quoted as saying:
“At the moment we do not have enough leaders. There’s a lot that the NHS can teach others but that doesn’t mean that we should be complacent. Look at what McDonald’s does. They start leadership at shift manager level. They drive leadership training through every level of their company. Restaurant managers learn how to develop a culture of continuous improvement, how to hold their teams and themselves accountable, and how to apply best practice for their outlet.”
If I were a National Health Service (NHS) Manager I’d probably be deeply offended at the notion that the complexity of leading and managing patient care services is somehow comparable with flipping burgers. McDonald’s might well have some good practice, but at a basic level, they only have one service offering: food. Some of their products can be customized, but you are heavily discouraged from doing this as the company prides itself in its efficiency.
Leading a team of people in such an environment, while stressful, is straightforward. The success KPIs are simple, as is line of sight of the employees on shift. The closest thing to an emergency that a leader of such a team will experience for the most part is too many customers waiting too long for their food and getting annoyed. Hardly life or death.
A manager in the NHS, meanwhile, operates with much higher stakes and competing demands.
If they are a clinician, then they might well have to step in to administer medical care. At this point, they have switched roles from leading people to having responsibility over others’ care and wellbeing, potentially in situations where the wrong call can lead to death of a patient. Even if they are non-clinicians, senior managers can hold the responsibility for deciding what action needs to be taken when an accident and emergency department has reached capacity. In that situation, patients might be rerouted to another hospital meaning emergency care could be delayed, a potentially life-threatening situation.
Within the professions, there are competing ideologies where patient treatment rubs up against cost considerations and where a clinician’s personal ethical boundaries and obligations are challenged, both legally and practically. No one in McDonald’s ever has to choose between extending someone’s life against the exponential cost increases that might occur as a result.
Building an Operating Model Template
At the highest level, the two organizations have very little in common. Of course, you can take learnings from one organization and apply them to another. However, I would suggest caution. I’ve lost count of the number of times I have been on the receiving end of a leader in an organization wishing to use benchmarks of other organizations to redesign their own. Benchmarking can be useful, particularly in a rewarding setting where the market is fluctuating, or you need to demonstrate an equal value pay defense, but in terms of your operating model template, it’s a waste of time.
The Uniqueness of Each Organisation
Each organization is unique. In addition to the differentiating factors of the NHS, it also has a difficult political narrative to satisfy. It must juggle demands to increase efficiency and decrease spending on inefficient activities with demands for patient-centered approaches to care. If you are in the business of designing an organization, you firstly need to decide how you want to service your customer base.
The NHS has a vast number of services. Many of these are routine non-emergency type offerings, for example, an MRI scan. The machinery is complex and does magical things, but the basic process is as follows:
- A referral is received
- A patient is called in for a scan
- The patient is put through the machine and there is a scan at the end
Here, the McDonald’s operating model works. No intervention other than running the program is needed. However, what if the scan shows an abnormality? In the case of cancer, for example, a specialist cancer service is needed. While the MRI service might have been highly efficient, it cannot switch to becoming customer intimate and start treatment of the cancer. There is a shift towards personalization of medical intervention at this point and the operating model template changes from that of McDonald’s.
One size does not fit all and across all of the cancer cases that are treated in a given year, your diagnosis may be rare and unlike most others.
In reality, the NHS is not a single organization. It comprises of countless organizations acting under a brand. For example, there are several distinct brand offshoots like ‘NHS England’ or ‘NHS Scotland’ that segment the organization by geography. These can be further broken down into smaller organizations. Making sweeping statements about the application of leadership practices from a fast-food company, such as from Health Secretary Hancock, isn’t valid in such a complex system. A better comparison would be a large complex multinational holding company with a number of separate but related businesses.
Organizations are by nature unique, you can incorporate learnings from others, but it is a dangerous game when it is done so without fully understanding the positioning of your own organization.
Your Gravitational Pull—Which Are King and Queen?
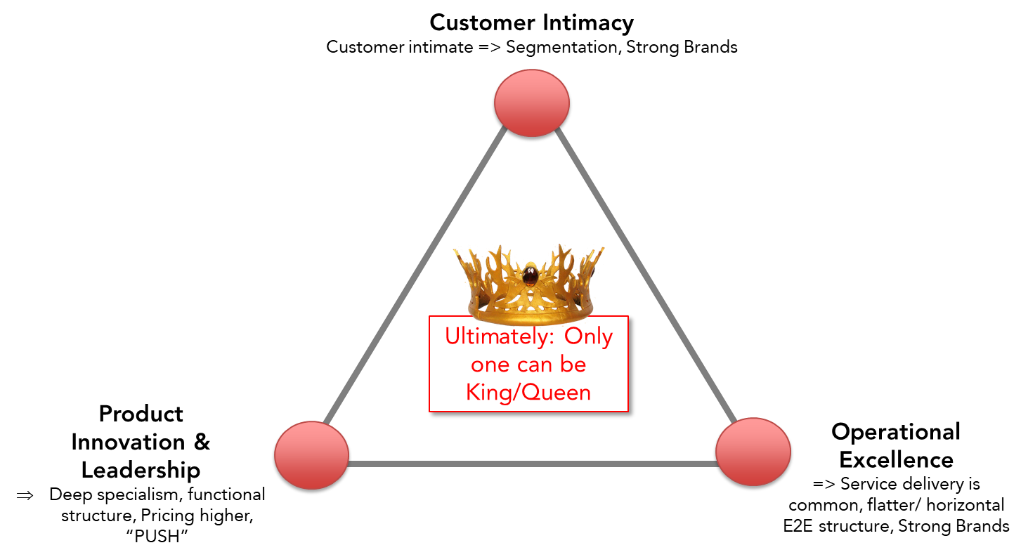
The first question a leader should ask when addressing an operating model is what is the organization’s gravitational pull, or focus value? This could be a focus on becoming operationally excellent, customer intimate or a product leader. While you will have a prioritized pull, one will ultimately take the role of King and the other Queen
In the case of the MRI Scanning service, Operational Excellence might well be correct. So, what might result? Well, if I am designing an operating model that is highly efficient, selecting this option would suggest then I am going to prioritize speed, repetitiveness, cost-efficiency. Simply put, I want to get as many patients through the scanning process in any given day as quickly, cheaply, and accurately as possible.
In the case of a cancer diagnosis and resulting demand for specialized care, the next part of the organization (possibly a different company) might be Customer Intimacy or Product Leadership. If it were a fairly routine case, then the service that is offered might be customer intimate. There could be a range of standardized options that the patient. The point is that while the overarching success measure will be remission, the ‘how’ is more bespoke and intimate to the particular customer.
What about if the cancer happened to be unique or maybe the regular treatments have failed? Here the patient might be referred to a leading expert in experimental or new treatments. At this point, the design choices changes to Product Leadership. The customer (patient) is seeking the newest or latest treatment available. It might well be a high cost and not many people have had it before. It might even be that the NHS has deemed the treatment too expensive or that it is offered elsewhere in the world. A grim scenario, but these are realities organizations and individuals face on a daily basis.
Conclusion
The overriding point is that comparing organizations is not as simple as identifying one company’s good practices and then copying and pasting over your organization. It is way, way more complex than this and needs proper and thorough design thinking throughout the value stream(s) in order to be successful. Cherry-picking and grandstanding? Let’s leave that to the politicians while the rest of us get on with real work.
Dr. Stuart Wigham was a Content Manager and Consultant at ON THE MARK.
OTM is the leading global boutique organization design consultancy with offices in the USA and UK. With over 450 successful redesigns and operating model modernizations completed, OTM is owner of the industry’s most integrated, comprehensive and holistic organization design solution. OTM enables its clients to realize their future ambitions.


